EADV 2019: Risk of osteoporosis and fractures with atopic dermatitis and steroid use
European Academy of Dermatology and Venereology Congress 2019
Most treatments routinely used for atopic dermatitis (AD) have been available for some time and newer therapies, such as dupilumab, are being continuously monitored for safety and possible adverse effects. Regular evaluation and review of disease pathophysiology and treatment-related adverse events in AD can improve physician awareness of less common or under-reported side effects, as well as potential outcomes that may have longer-term implications on patient health.
At the 28thAnnual Congress of the European Academy of Dermatology and Venereology (EADV), held 9-13 October 2019 in Madrid, Spain, researchers presented new data from a retrospective population-based study examining the risk of osteoporosis and major osteoporotic fractures in Danish adult patients with AD.1 In this week’s commentary, we present their findings.
Risk associated with atopic dermatitis
A population-based cohort study conducted in the UK recently concluded that people with atopic eczema have increased fracture risk, particularly major osteoporotic fractures.2 There are several factors associated with AD that may predict altered risk of osteoporosis and major osteoporotic fractures in adults with the disease (Figure 1).
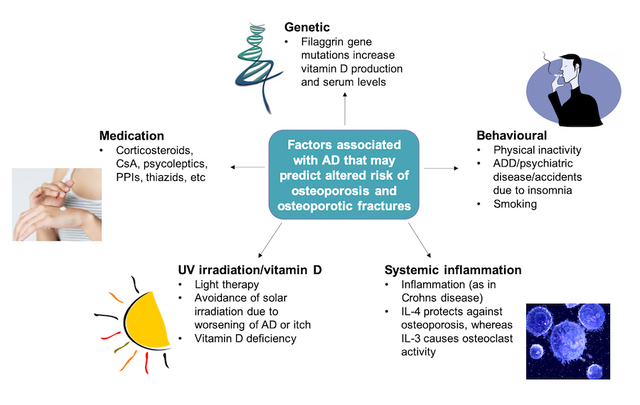
Figure 1. Factors that may predict altered risk of osteoporosis and osteoporotic fractures.
AD, atopic dermatitis; ADD, attention deficit disorder; CsA, cyclosporin A; IL-, interleukin; PPI, proton pump inhibitor.
To assess the risk of osteoporosis and major osteoporotic fractures in adults with AD, a retrospective analysis included all Danish adults (>18 years) in the National Patient Registry and National Prescription Registry from 1997 to 2017. Patients with AD were matched 1:10 with controls (sex and age), and those with a diagnosis of osteoporosis and those treated with osteoporosis medication prior to the index date with excluded. Researchers conducted separate analyses using topical corticosteroids (TCS) and topical calcineurin inhibitors (TCI).
Risk of osteoporosis and fractures with atopic dermatitis and steroid use
The investigators included 10,636 adults with AD and 87,989 matched reference individuals. The mean age (± standard deviation [SD]) was 36.6 years (± 15.0) and 63.9% were female. Although the two groups were evenly matched by patient demographics and characteristics, there was a higher proportion of asthma sufferers among AD individuals (13.4%) relative to the general population control group (2.8%). There was also more systemic corticosteroid (22.6% versus 3.5%), cyclosporine A (0.9% versus 0.03%), proton pump inhibitors (3.8% versus 2.3%) and psycholeptic (13.3% versus 10.5%) use among individuals with AD.
The absolute risk of endpoints if 10,000 individuals were followed for 1 year was higher with AD relative to the general population, and higher in people with AD and previous systemic steroid use (Table 1).
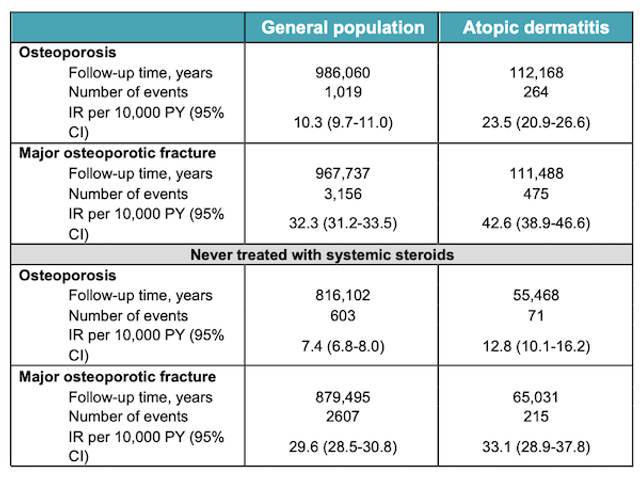
Table 1. Absolute risk of endpoints if 10,000 individuals are followed for 1 year.
CI, confidence interval; IR, incidence rate; PY, person-years.
The fully adjusted risk of study outcomes, adjusted for age, gender, body mass index (BMI), socioeconomic group, asthma and oral medication use, consisted of a hazard ratio (HR) of 1.51 (95% confidence interval [CI], 1.29 to 1.75) and HR of 1.18 (95% CI, 1.07 to 1.31) for osteoporosis and major osteoporotic fractures, respectively, in the entire population, and a HR of 1.82 (95% CI, 1.46 to 2.28) and a HR of 1.14 (95% CI, 1.06 to 1.23) for osteoporosis and major osteoporotic fractures, respectively, in individuals who had never used systemic corticosteroids.
The fully-adjusted risk of study outcomes with TCS and TCI showed that the risk of osteoporosis is increased with potent and very potent TCS and there is also an increased risk of major osteoporotic fractures with very potent TCS (Table 2).
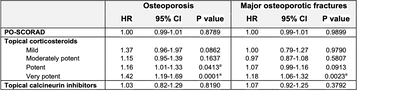
Table 2. Fully-adjusted risk of study outcomes with topical steroids and calcineurin inhibitors.
CI, confidence interval; HR, hazard ratio; PO-SCORAD, Patient-Orientated Scoring Atopic Dermatitis.
aSignificant P value.
The findings from this study indicate there may be an increased risk of osteoporosis and major osteoporotic fractures in people with AD. Further research is needed to confirm and quantify the risk in AD patients who use potent and very potent TCS. As chemical penetration is increased in AD skin, the researchers concluded that dermatologists should consider alternative treatments in chronic excessive users of TCS.
Action Eczema
To find out more about the mechanisms of action and use of established and emerging topical and systemic therapies in adult patients with AD, explore our online CME courses:
To test your knowledge of eczema treatment and management as part of patient-centred care, try our ‘Self-assessment in atopic dermatitis’ and ‘Case challenge: 48-year-old woman with conjunctivitis during treatment’ modules.
Interested in reading more about the AD research presented at EADV this year? Sign up to Action Eczema and be notified when our EADV 2019 Congress Report is available online for viewing and CME credit.
References
- Thyssen JP. Risk of osteoporosis and major osteoporotic fractures in adults with AD. Presented at the European Academy of Dermatology and Venerology (EADV) 2019. 9-13 October 2019; Madrid, Spain. Oral session.
- Lowe KE, Mansfield KE, Delmestri A, et al. Atopic eczema and fracture risk in adults: A population-based cohort study. J Allergy Clin Immunol. 2019; S0091-6749(19):31251-31255.